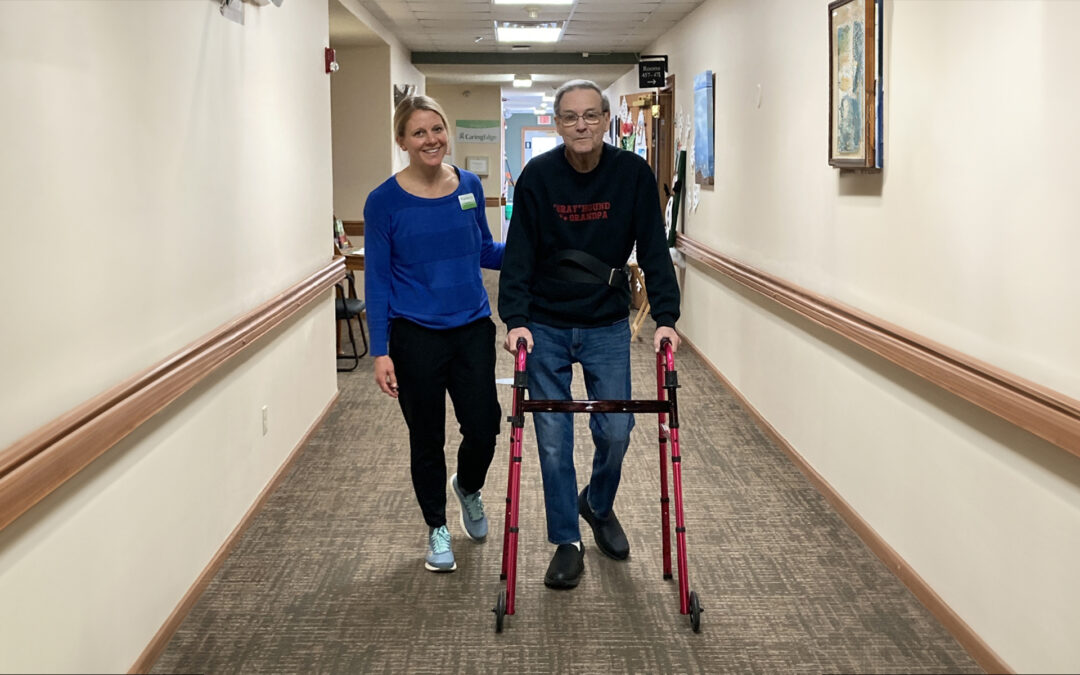
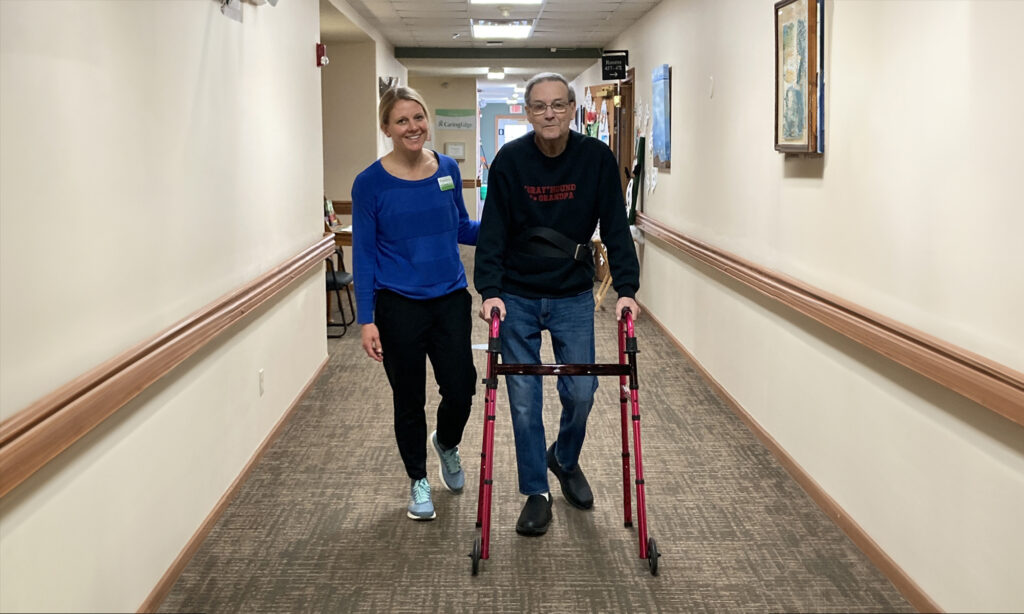
Get Some “Spring” in Your Step!

Perhaps you’ve had a recent fall or a near miss or didn’t move as much as you would have liked this winter. Aging, injuries, stiffness, and being cooped up indoors can slow us down. The good news is there’s room to improve!
Did you know that walking speed can predict the future of your independence? Research shows that the slower someone walks, the more likely they are to have difficulty with tasks of daily living, more likely to have falls, and more likely to be hospitalized! This is astounding information, and many don’t realize that gait speed can be tested and improved.
What is Gait Speed?
How fast someone walks.
A Gait Speed Evaluation Can Predict:
- The risk of future falls
- If assistance may be needed with tasks of daily living/personal care
- Life expectancy
Why Complete a Gait Speed Analysis?
If you’re falling, losing balance, or you’ve started to slow down, the test may help indicate if you’re at risk for further decline. It can help your healthcare providers create a plan of care to help you improve. Sometimes, the plan can include outpatient therapies along with the recommendation for having help with tasks of daily living to reduce your risk for further decline.
How Long Does the Test Take?
Under five minutes!
What do I have to do?
Walk as usual for a short distance while you’re observed by clinical staff.
Gait Speed Analysis by CaringEdge:
Our physical therapists can offer a gait-speed analysis evaluation. Depending on the results, you could be eligible for regular and routine physical therapy. Physical therapy has been proven to improve independence and safety and, ultimately, enhance your quality of life!
A free gait speed analysis can provide a consistent, reliable, and statistically relevant way to track and prevent falls and calculate the risk for further decline. The scores can also be documented as a data point that we can re-screen regularly to monitor the residents’/patients’ mobility, safety, and risk level with functional mobility.
Demystifying Gait Speed:
Many seniors feel that they have to slow down when they walk. While this rings true when walking on icy or uneven surfaces, it’s not so true for walking around your home daily to complete the tasks you need. The slower seniors walk around their homes, the more likely they will have a trip or a fall.
We say it often: you lose it if you don’t use it. A gait speed analysis can be a great starting point to help you get back to doing the things you want to be doing again. We’d happily meet with you, assess your condition, learn your goals, and create a care plan. Best of all, we accept Medicare for our home health services! Therapies can typically be covered to keep out-of-pocket costs minimal or completely erased.
Your future is now! Let CaringEdge’s therapists and home health get you back to feeling your best. Reach out to us today at info@caringedge.com.